Tongue-tie (ankyloglossia) is a condition in which the thin piece of skin under the baby’s tongue (the lingual frenulum) is abnormally short and may restrict the movement of the tongue.
Tongue-tie occurs in about three per cent of babies and is a condition that can run in families. It is more commonly found in boys.
Impact of tongue-tie
The most immediate impact of a tongue-tie is on a baby’s ability to breastfeed effectively. It may interfere with a baby’s ability to latch and suckle at the breast leading to:
- nipple pain and trauma
- poor breast milk intake
- a decrease in milk supply over time.
Tongue-tie may also have an effect on oral hygiene. Its effect on speech development remains controversial.
A procedure to release a tongue-tie may be recommended if it is impacting on breastfeeding.
The procedure is called a lingual frenotomy. Before preforming this procedure clinicians who work with breastfeeding mothers and their babies will assess the baby’s mouth, breastfeeding and maternal comfort.
If breastfeeding is painful, there is poor milk transfer and there is significant tongue-tie, release will improve the baby’s ability to breastfeed.
Sometimes a tongue-tie causes no problems with breastfeeding and requires no action.
Health professionals seeking further information please see the Women’s Clinical Guideline Assessment and management of babies with tongue-tie
Signs of a significant tongue-tie
- Tongue cannot extend beyond the baby’s lips.
- Tongue cannot be moved sideways.
- Tongue tip may be notched or heart-shaped.
- When the tongue is extended, the tongue tip may look flat or square instead of pointed.
- Breastfeeding problems such as:
- nipple pain and damage
- a misshapen nipple after breastfeeding
- a compression/stripe mark on the nipple after breastfeeding
- the baby often loses suction on the breast whilst feeding
- a clicking sound may be heard while the baby is feeding
- poor weight gains.
Assessment
A lactation consultant or experienced clinician will conduct a thorough assessment of breastfeeding and baby’s tongue mobility to determine if release is required.
If the frenulum is thin and the baby is less than around four months of age, the frenulum can be released as an outpatient procedure without any anaesthesia. A baby who is older or who has a tongue-tie that is thick, may need to be referred to an appropriate specialist.
Tongue-tie release
Babies should have had Vitamin K at birth (or at least 2 oral doses) before the tongue-tie release is considered.
It is preferable for the tongue-tie to be released prior to a feed. If your baby is due to have this procedure please try not to feed your baby for at least one hour before your appointment.
The release of a tongue-tie involves the clinician placing a finger and thumb under the baby’s tongue to gain clear access to the frenulum. The frenulum is released with a small pair of sterile scissors.
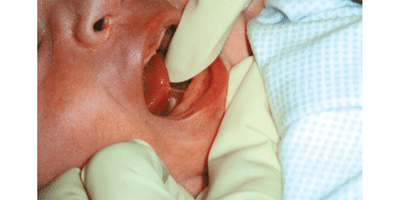
A drop or two of blood at the release site is normal and is rarely a problem. Some babies may be unhappy at being held still and having fingers placed in their mouth. Occasionally a baby will startle when the release is performed but will settle quickly once comforted. Following the procedure, the mother will be encouraged to breastfeed straight away.
Possible complications of the procedure are bleeding (usually minimal) or infection (extremely rare). There is no special care required following the procedure. Occasionally, during the healing process a small white patch may be seen under the tongue of some babies. This is normal and should resolve within two weeks of the release.
If your baby has a tongue-tie release and you have any concerns following the procedure, please contact your lactation consultant, maternal and child health nurse, paediatrician or your local doctor.
Related information
- Australian Breastfeeding Association 24 Helpline - 1800 686 268
- Maternal & Child Health Line 24 hour Helpline - 13 22 29
- Provide feedback about the information on this page
Related Health Topics
Disclaimer
The Women’s does not accept any liability to any person for the information or advice (or use of such information or advice) which is provided on the Website or incorporated into it by reference. The Women’s provide this information on the understanding that all persons accessing it take responsibility for assessing its relevance and accuracy. Women are encouraged to discuss their health needs with a health practitioner. If you have concerns about your health, you should seek advice from your health care provider or if you require urgent care you should go to the nearest Emergency Dept.