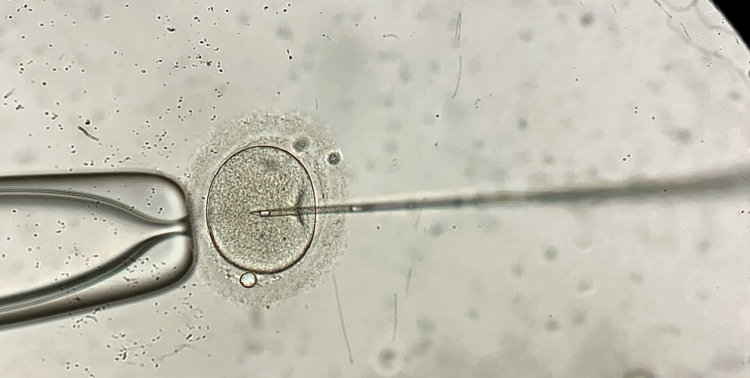
Research conducted at the Royal Women’s Hospital has found that many Australian women are opting to purchase IVF treatment add-ons, such as acupuncture and herbal medicine, in an effort to improve their chances of having a baby.
The study, published in the journal Human Reproduction, was conducted by researchers from the Women’s, the University of Melbourne, Queensland University of Technology, the University of Manchester, Monash University, and the Victorian Assisted Reproductive Treatment Authority.
It included 1,590 Australian women and found 82 per cent had used one or more add-ons when going through IVF in the past four years. Most of these optional extras (72 per cent) came with an additional cost.
Add-ons are defined as procedures, techniques or medicines that are used in addition to standard IVF protocols. They include additional medications; complementary and alternative medicines such as acupuncture; technology such as time lapse imaging of embryos; and procedures including ‘endometrial scratching’.
Many of these add-ons lack evidence to show they are safe and effective.
With 75,000 IVF cycles completed every year in Australia, and with more affordable IVF services available in Victoria, the lead researcher Dr Sarah Lensen says there is a strong need to better understand the whole IVF experience in Australia, as well as the treatment options people choose and why.
“Assisted reproductive technology really has come so far. But, as researchers, we still have fundamental questions about the experience of people going through IVF,” says Dr Lensen.
“When people face fertility challenges, they are often in the vulnerable position of not having a full understanding of what treatments are available to them, what they involve and what the chances of the treatments resulting in a baby for them really are. It is complex, and it’s often a steep learning curve.
“It’s important that we build up a solid evidence base so we can help inform those providing IVF and those going through it themselves with key information. We know the IVF journey isn’t always easy, so we hope this information will improve the experience.”
“The Women’s is one of the few places that has low-cost IVF available to patients, but at many private clinics the cost of fertility treatments can be very high – especially when extra medications, and additional testing is involved,” says Dr Lensen.
“There often isn’t high-quality evidence to support these add-ons in routine practice. Hopefully, this will improve our understanding and inform decision-making in the future.”
Read related content from the Women's
-
 40 years since the first IVF baby was born at the Women’s
40 years since the first IVF baby was born at the Women’sWe celebrate 40 years since the birth of Australia’s first baby conceived through IVF, Candice Reed – a major milestone for science and fertility.
Learn more -
 IVF success comparator welcomed by the Women’s
IVF success comparator welcomed by the Women’sThe Royal Women’s Hospital has today welcomed a new online portal enabling women and families to compare Australian IVF clinic success rates and helping them predict IVF success based on age, infertility diagnosis and other factors.
Learn more -
 Study aims to improve the IVF experience for Australians
Study aims to improve the IVF experience for AustraliansA new research project at the Royal Women’s Hospital will investigate the experience of having IVF in Australia – and hopes to identify it can be improved for people undergoing IVF in the future.
Learn more